Getting a molar pregnancy diagnosis when you were hoping for a healthy baby is heartbreaking. But here's what we want you to know right away - this is not your fault, and you are not alone. A molar pregnancy is a rare pregnancy complication, occurring in just 1 in every 1,000 pregnancies, and most people who go through it go on to have healthy pregnancies afterwards.
So what is a molar pregnancy? In the simplest terms, the meaning of a molar pregnancy is this: a fertilisation error causes abnormal tissue to grow in the uterus instead of a healthy placenta and baby. That's the definition of a molar pregnancy, and while it sounds scary, it is completely treatable.
At One World Fertility, we're here to guide you through every step - with honest answers, warm support, and expert care.
What Exactly Is a Molar Pregnancy?
During a healthy pregnancy, very small cells known as trophoblasts grow and finally make the placenta, which feeds your baby. But sometimes, these cells don't act right because of a mistake in the DNA when they were fertilised. They don't make a healthy placenta; instead, they grow in a weird way and fill the uterus with a bunch of gas-filled sacs. A molar pregnancy, also known as a hydatidiform mole, is what that lump is.
Gestational trophoblastic disease (GTD) is a more general term for molar pregnancy. It is a group of situations where abnormal trophoblastic tissue grows in the uterus. Usually, this molar pregnancy tissue turns into a growth that is not cancerous. There is a small chance that a molar pregnancy tumour is not dangerous, even though the word "tumour" can make you feel scared.
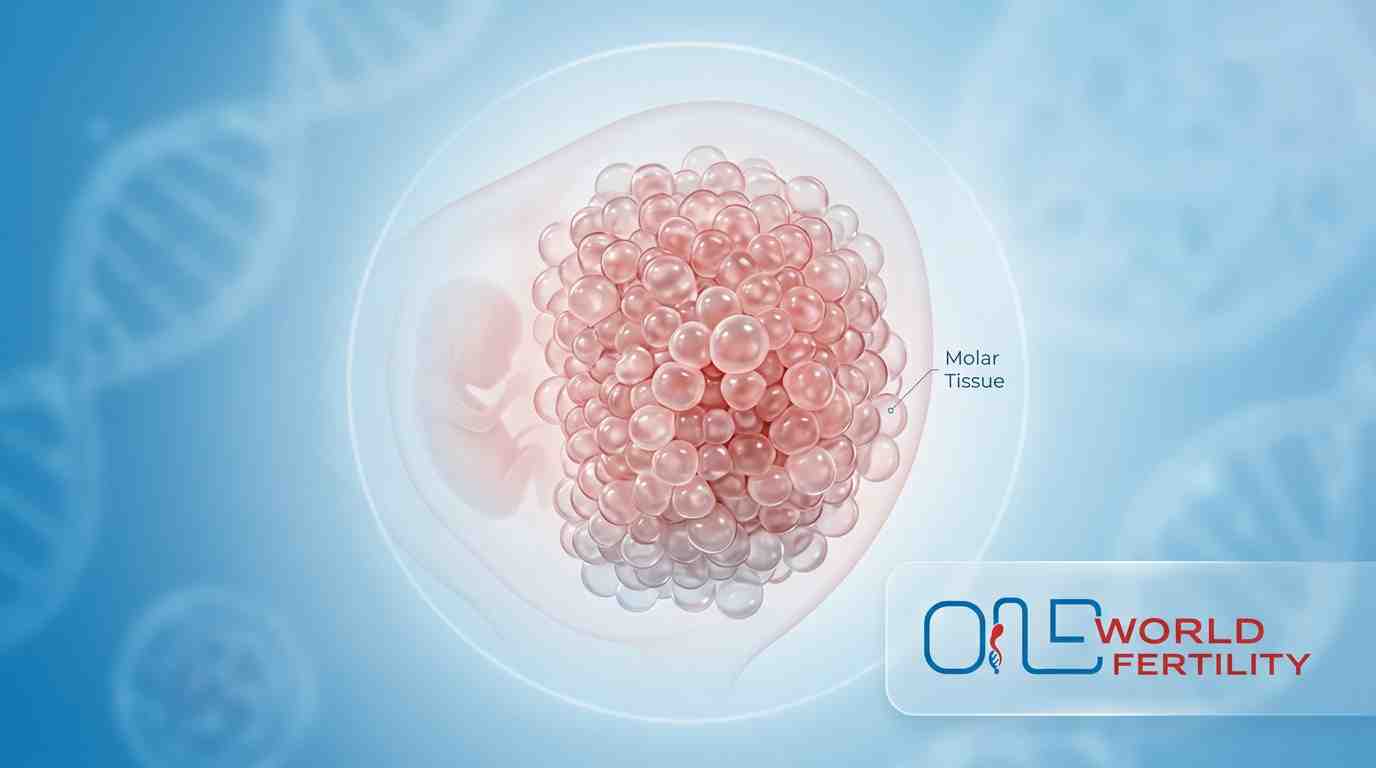
What Does Molar Pregnancy Tissue Actually Look Like?
Visually, the abnormal tissue forms grape-like cysts - small, round, fluid-filled sacs clustered together. These grape-like cysts in molar pregnancy are what give it its distinctive appearance on ultrasound, and in some cases, they may even pass through the vagina, which is one of the earliest warning signs.
Is a Molar Pregnancy the Same as a Tumour?
In a sense, yes - but not the kind most people fear. Molar pregnancy cysts are benign (non-cancerous) growths in the uterus. The hydatidiform mole's meaning, at its core, is simply an abnormal pregnancy where placental tissue grows out of control. It isn't a tumour pregnancy in the traditional cancer sense - though in rare cases, it can progress to a more serious condition, which we'll cover later in this guide.
Types of Molar Pregnancy - Complete vs Partial Explained
Not all molar pregnancies are the same. There are two types of molar pregnancy, and understanding the difference matters - both for treatment and for knowing what to expect. Whether it's a complete or partial molar pregnancy, both require prompt medical care, but they differ in how they form, what they look like, and the level of risk involved.
What Is a Complete Molar Pregnancy?
When a sperm fertilises an empty egg, one that doesn't have any genetic material from the mother, this is called a complete molar pregnancy. There is no baby because the egg is empty. There are 46 chromosomes that are only from the father because either two sperm fertilise the same egg, or the father's chromosomes duplicate. Instead of a placenta or baby, the uterus fills with strange, fluid-filled tissue.
There are more problems that can happen during a full molar pregnancy. One of these is chronic gestational trophoblastic neoplasia (GTN), and in very rare cases, choriocarcinoma. Also, compared to partial molar pregnancies, they have a slightly higher risk of happening again.
What Is a Partial (Incomplete) Molar Pregnancy?
When two sperm fertilise one regular egg, you have a partial molar pregnancy, which is also known as an incomplete molar pregnancy. Because of this, the baby has 69 chromosomes instead of the normal 46, which means it has an extra set of chromosomes from the father. Sometimes, a fetus may start to grow, but it can't live because of a serious chromosomal imbalance.
A partial mole is usually seen as less dangerous than a full molar pregnancy. The chance of getting cancer is smaller, and problems can still happen, but they happen less often. Even so, it still needs the same careful care and tracking afterwards.
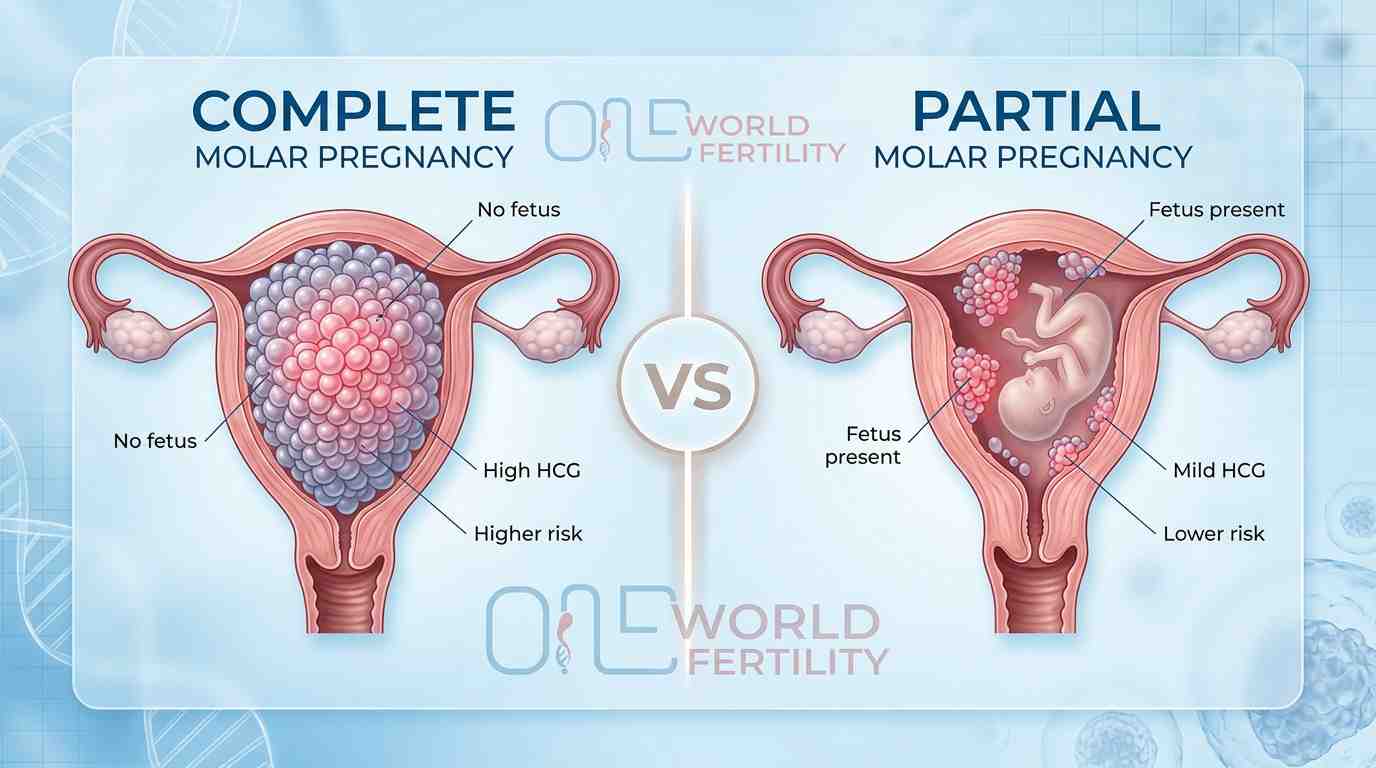
Complete Molar Pregnancy vs Partial Molar Pregnancy - Key Differences
Feature
|
Complete Molar Pregnancy
|
Partial Molar Pregnancy
|
Fetus present?
|
No
|
Sometimes (cannot survive)
|
Chromosomes
|
46 (all paternal)
|
69 (extra paternal set)
|
HCG levels
|
Very high
|
Mildly elevated
|
Cancer risk
|
Higher
|
Lower
|
GTN risk
|
15–20%
|
Up to 5%
|
How Does a Molar Pregnancy Happen? (Causes & Pathophysiology)
If your first question after a diagnosis is "why did this happen to me?" - that's completely understandable. Here's the most important thing to know: a molar pregnancy is caused by a random genetic error at fertilisation. Nothing you did caused this.
What Causes a Molar Pregnancy?
In a healthy pregnancy, both the sperm and the egg add 23 chromosomes to the embryo. In a molar pregnancy, that process goes wrong. When a woman is pregnant with her first child, the egg is empty, so all of the genes come from the father. There are 69 chromosomes instead of 46 in a partial molar pregnancy because two sperm fertilise one egg. In either case, the chromosomal imbalance makes it impossible for a healthy birth to happen. The only thing that can cause a molar pregnancy is genes. It has nothing to do with your lifestyle, food, or anything else you can change.
Molar Pregnancy Pathophysiology - What Happens Inside the Uterus?
Instead of forming a healthy placenta, the trophoblast cells multiply abnormally and create a mass of fluid-filled sacs. What makes this confusing for many women is that the abnormal molar pregnancy tissue keeps producing HCG - the pregnancy hormone -which is why you still feel pregnant and get a positive test. Your body isn't lying to you; it's just responding to faulty signals from the molar pregnancy placenta.
Signs and Symptoms of Molar Pregnancy
When they first find out they have a molar pregnancy, many women think everything is fine. That's why it's so upsetting when they are told the truth. The early signs of a molar pregnancy can look a lot like those of a healthy early pregnancy. It's very important to know what to look out for.
Early Molar Pregnancy Symptoms (First Trimester)
During the first three months of pregnancy, the most common signs are:

- Vaginal bleeding: different shades of brown to bright red
- Severe nausea and vomiting: More often than not, it's worse than normal morning sickness
- Grape-like cysts passing from the vagina: one of the most important signs
- Pain or pressure in the pelvis
- Abnormally high HCG levels: found in blood tests
Should you notice any of these signs of a hydatidiform mole, you should call your doctor right away.
Molar Pregnancy Symptoms at 5 Weeks - What to Watch For
Can a molar pregnancy be detected as early as 5 weeks? Most of the time, yes. At 5 weeks, these signs of a molar pregnancy can easily be mistaken for those of a normal early pregnancy: tiredness, nausea, and a positive test. But at this point, vaginal bleeding for no reason is generally the first sign of trouble. If you start bleeding in the early stages of pregnancy, you should always get it checked out. At 5 weeks, a blood test that shows HCG levels that are higher than normal may also be the first sign of a molar pregnancy.
Signs of Molar Pregnancy That Come Later or Less Often
If you don't catch a molar pregnancy early, these other signs may show up:
- The uterus is growing faster than usual for the stage of pregnancy.
- Having high blood pressure before 20 weeks is called preeclampsia.
- Lymph nodes
- Signs of hyperthyroidism (fast heartbeat, nervousness, tremors)
- Anaemia, or not having enough iron
Not many people have these hydatidiform mole signs, but it's important to know them, especially if you haven't had your regular scans yet.
Molar Pregnancy Bleeding -What Does It Look Like?
Bleeding in a molar pregnancy is usually the first sign that something isn't right. There may be light spots or heavy blood, and the colour may range from dark brown to bright red. Unlike normal implantation spotting, molar pregnancy discharge may also contain small cysts that resemble grapes. This is a clear sign that you need to see a doctor right away.
When should you see a doctor? Any blood in the uterus during pregnancy should be reported. But don't wait-go in right away if you start to bleed and have severe vomiting, pelvic pain, or pass any strange tissue.
Molar Pregnancy HCG Levels - What the Numbers Mean
One of the most telling clues in a molar pregnancy diagnosis is the HCG level. If your doctor told you that your HCG level was too high, here's why and what it means.
Why Are HCG Levels So High in Molar Pregnancy?
HCG - the pregnancy hormone - is normally produced by a healthy placenta. When there is a molar pregnancy, the abnormal trophoblastic tissue steps in and makes too much HCG. Because of this, the HCG levels are very high, much higher than what you'd expect at any time of a normal pregnancy. In fact, this is one reason why a molar pregnancy is sometimes thought to be happening before an ultrasound is done.
Molar Pregnancy HCG Levels Chart (by Week)
Week
|
Normal HCG Range (mIU/mL)
|
Molar Pregnancy HCG (Approximate)
|
4 weeks
|
10 – 750
|
Often > 100,000
|
6 weeks
|
1,080 – 56,500
|
Often > 200,000
|
8–10 weeks
|
7,650 – 229,000
|
Abnormally persistent / rising
|
Important note: Molar pregnancy HCG levels don't follow the normal doubling pattern. Instead of peaking and then gradually declining, they may keep rising or stay stubbornly elevated - which is a key warning sign your doctor will watch for.
At 4 weeks and 6 weeks, molar pregnancy HCG levels are often ten times or more higher than usual. This is one of the earliest and most accurate signs that a woman is pregnant with a molar.
HCG Monitoring After Molar Pregnancy Treatment
Treatment doesn't end with the removal of molar tissue. What's important is that your doctor will closely monitor your HCG levels after surgery. Once the treatment is over, HCG must go back to zero. This proves that all the abnormal tissue was safely removed. Blood tests are usually done once a week until the HCG level drops to zero, then once a month for 6–12 months.
If HCG levels go up again or don't go down after treatment, it could be an early sign of prenatal trophoblastic neoplasia (GTN), which means that some molar tissue may still be working. This is exactly why follow-up is so important-HCG tracking can catch this early, and your care team will stay in close touch with you during this time.
How Is a Molar Pregnancy Diagnosed?
Most molar pregnancies are caught early - often during a routine first-trimester check-up. Here's how doctors confirm the diagnosis.
Molar Pregnancy Ultrasound - What Doctors Look For
The first and most important step is to get an ultrasound. Doctors look for these things on a molar pregnancy ultrasound:
- A "snowstorm" look, which is a whirling, grainy pattern caused by damaged tissue
- Instead of a healthy placenta, there are sacs full of fluid
- In a full-molar pregnancy, there is no movement from the fetus.
These scan results are usually a reason to be worried right away.
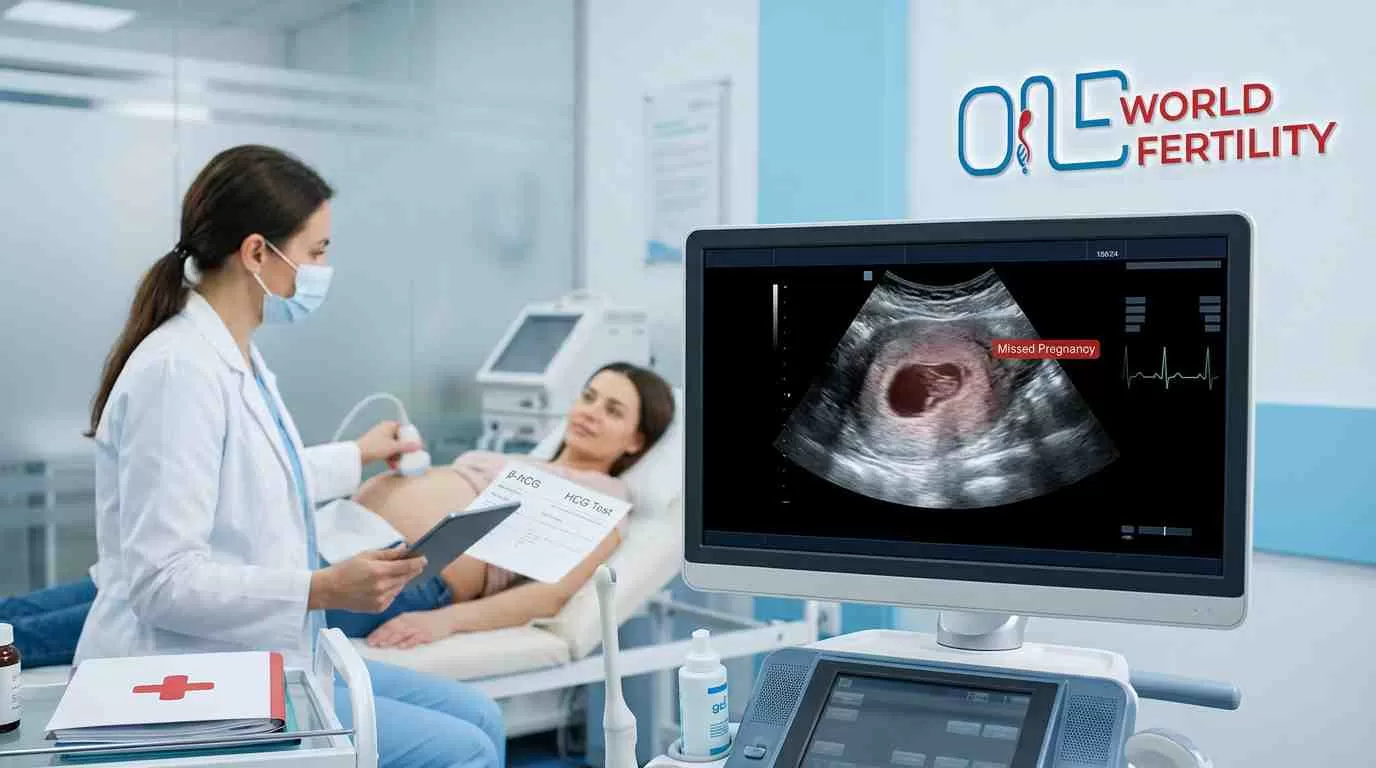
Molar Pregnancy Ultrasound Pictures - What It Looks Like
On a molar pregnancy image, the uterus looks like it's full of a lumpy, uneven substance that looks more like a group of tiny air bubbles than a usual pregnancy sac. There is no clear form to the baby, and in full molar pregnancies, there is no embryo. An ultrasound can often detect pregnancy as early as 8–10 weeks.
Blood Tests for Molar Pregnancy
The following will also be checked in your blood by your doctor:

- Abnormally high HCG levels: Way past the normal ranges for pregnancy
- Thyroid function: Hyperthyroidism can sometimes be caused by molar pregnancies.
- Complete blood count: to see if they have anaemia
How Early Can a Molar Pregnancy Be Detected?
- This is usually done during the first stage, which lasts from 8 to 12 weeks.
- If HCG levels are unusually high, fears can start as early as 5–6 weeks.
- Getting pregnancy care early is important to catch it early.
Molar Pregnancy Treatment Options
A molar pregnancy won't go away on its own, but the treatment is easy, works, and usually won't affect your ability to have children in the future. This is what you can expect.
Dilation and Curettage (D&C) - The Standard Treatment
For a molar pregnancy, a molar pregnancy D&C is the best way to treat it. A small suction device is used to remove all the unwanted tissue from your uterus after your cervix is gently opened. Because it's done under general anaesthesia, there is no pain during the process. After that, it's normal to have some light cramps and spotting for a few days. Most women are back to normal within a week.
When Is a Hysterectomy Recommended?
For most women, D&C is all that's needed. A hysterectomy is only considered when:
-
The tissue is deeply invasive and D&C isn't enough
- The woman does not wish to conceive again
- Complication risk is significant
-
It's a rare step - not the norm.
Post-Treatment HCG Monitoring
After treatment, your HCG levels are monitored closely to confirm all tissue has been removed.
Monitoring Phase
|
Frequency
|
After treatment
|
Weekly blood tests
|
Once HCG reaches zero
|
Monthly checks
|
Total duration
|
6–12 months
|
Pregnancy should be avoided during this entire period - a new pregnancy would make it impossible to track whether molar tissue has returned.
RhoGAM Injection - Who Needs It?
If you have an Rh-negative blood group, you'll receive a RhoGAM injection after treatment. It's a simple, routine precaution to protect future pregnancies from antibody complications. Just make sure your care team knows your blood type.
Molar Pregnancy Complications - What Can Go Wrong?
Most pregnancies in the molars are treated properly and don't cause any long-term problems. But you should know what can happen if you wait too long to get treatment or if molar tissue stays after the molar tissue are taken out. That way, you'll know exactly what to look out for.
What Is Gestational Trophoblastic Neoplasia (GTN)?
Even after a D&C goes well, there are times when small amounts of molar tissue stay in the uterus and keep growing. This is known as a GTN pregnancy, which stands for fetal trophoblastic neoplasia. It can turn into an invasive mole, meaning the tissue grows deeper into the uterine wall.
The good news? GTN is very easy to treat; most of the time, treatment works, but sometimes a hysterectomy is needed. This is exactly why HCG tracking is done after treatment: to find any leftover tissue quickly.
Can a Molar Pregnancy Cause Cancer?
This is one of the most common - and most worrying - questions people ask. A molar pregnancy can sometimes turn into choriocarcinoma, which is a type of cancer. Even though it can spread to other organs, the most important thing to know is that choriocarcinoma reacts very well to chemotherapy and can be cured very often, even if it is found later. Can getting a molar pregnancy lead to cancer later in life? There is a chance of this happening, but it doesn't happen very often. After treatment, regular HCG tracking is meant to find any signs of this early.
Other Complications to Know
While uncommon, other molar pregnancy complications include:
- Uterine infection or sepsis - if tissue is left untreated
- Preeclampsia - dangerously high blood pressure
- Shock - a severe drop in blood pressure requiring urgent care
Is a molar pregnancy dangerous? It can be - but only when left untreated. With prompt diagnosis and proper follow-up, the overwhelming majority of women come through this safely.
Molar Pregnancy Risk Factors - Who Is at Higher Risk?
One can get a molar pregnancy at any time. But some things make it more likely. It's not about who's to blame if you know your molar pregnancy risk factors. It's about staying informed and ahead of the game.

The main dangers of molar pregnancy are:
- Age: A little more likely to happen to women under 20 or over 40
- Previous molar pregnancy: If you've had one before, your risk goes up.
- Two or more prior miscarriages: having a history of losing babies can be a factor
- Asian descent: According to statistics, the number of molar pregnancies is a little higher in some Asian groups.
Also, just to be clear, this wasn't caused by your lifestyle, food, stress, or anything else you did while you were pregnant.
Can a Molar Pregnancy Recur?
This is one of the first things women want to know after going through a molar pregnancy - could it happen again? The truth is that a molar pregnancy can happen again, but it doesn't happen very often. There is a one-in-one-hundred chance of having another molar pregnancy after the first one. If you've already had two molar pregnancies, that risk does go up. If that's the case, you should definitely talk to a genetic counsellor before trying to get pregnant again.
There is a small chance that a molar pregnancy will happen again, and most women who get early prenatal care and close tracking go on to have healthy pregnancies.
Can You Have a Twin with a Molar Pregnancy?
It seems very unlikely, but it can happen. A twin molar pregnancy is very uncommon. In this case, one twin develops properly while the other is a molar mass. Not more than 1 in 100,000 births are affected by it.
When a molar pregnancy with twins is proven, the healthy fetus in the molar pregnancy is in very real danger. As the molar mass keeps growing, the HCG levels rise dangerously, which makes problems like bleeding and hypertension worse for the mother.
An expert team handles each case of twin molar pregnancy on its own. Some are closely monitored, while others need to be addressed sooner to protect the mother. It's a very tough situation, and if you're going through it, please know that getting professional help from the start makes all the difference.
Twin Molar Pregnancy - Key Facts at a Glance
Factor
|
Details
|
How rare is it?
|
Fewer than 1 in 100,000 pregnancies
|
What happens?
|
One normal fetus + one molar mass develop together
|
Risk to mother
|
High HCG, preeclampsia, bleeding
|
Risk to healthy fetus
|
Limited survival chances due to complications
|
Management
|
Individual assessment by a specialist team
|
Pregnancy After Molar Pregnancy - What to Expect
If you're asking, "Will I ever have a healthy baby after this?" - the answer, for most women, is yes. Pregnancy after a molar pregnancy is absolutely possible, and the outlook is genuinely hopeful.
When Is It Safe to Try Again?
Most doctors recommend waiting 6 months to 1 year before trying to conceive. This is simply to allow your HCG levels to return to zero and stay there - because a new pregnancy would make it impossible to monitor for molar pregnancy recurrence. Once your doctor gives the green light, there's no medical reason you can't try again.
What to Expect in Future Pregnancies
When you do conceive again, your care team will recommend:
- Early ultrasound to confirm a healthy pregnancy
- Regular HCG monitoring in the early weeks
- Close prenatal follow-up for peace of mind
The risk of factor is low - around 1 in 100. Most women go on to have completely healthy pregnancies.
You Don't Have to Do This Alone
A molar pregnancy is a loss - and it's okay to grieve it. Take the time you need, lean on the people around you, and don't rush yourself emotionally.
At One World Fertility, we're with you beyond the diagnosis -through monitoring, fertility support, and every hopeful step toward your next pregnancy.
Your Fertility Future Is Not Defined by This
A molar pregnancy is frightening - but it is not the end of your story. It is manageable, it is treatable, and with the right care, most women go on to build the families they've always dreamed of. You did nothing to cause this, and you have every reason to hold onto hope.
Whatever stage you're at - whether you've just been diagnosed, are in the middle of treatment, or are thinking about trying again - you don't have to figure it out alone.
At One World Fertility, our specialists are here to guide you through every step. From diagnosis and treatment to HCG monitoring and future pregnancy planning, we offer the expert care and the human support that this journey deserves.
Ready to take the next step?
Consult with our fertility specialists today -mbecause your journey to parenthood deserves the very best care.
Book Your Consultation with One World Fertility
Frequently Asked Questions
HCG levels are usually much higher than normal pregnancy levels:
Often exceed 100,000 mIU/mL early on
Continue rising abnormally instead of stabilizing
Monitoring HCG levels helps doctors track recovery and ensure no molar pregnancy tissue remains.
In some cases, yes. Around 15–20% of complete molar pregnancies can develop into gestational trophoblastic neoplasia (GTN), a treatable form of cancer if detected early.
Complete molar pregnancy: No fetus, only abnormal tissue
Partial molar pregnancy: Abnormal fetus + molar tissue present
Both require medical management, but complete molar pregnancies carry a higher risk of complications.
Yes, it can be if untreated. Risks include:
Very high HCG levels
Heavy bleeding
Early preeclampsia
Rare progression to gestational trophoblastic disease (GTD)
Early treatment significantly reduces these risks.
It happens due to abnormal fertilization:
Complete molar pregnancy: No maternal DNA, only paternal genetic material
Partial molar pregnancy: Extra paternal chromosomes, often with a non-viable fetus
This explains how molar pregnancy happens and why these pregnancies cannot develop normally.
Bleeding is often dark brown or bright red and may include grape-like tissue. It can be heavier than normal pregnancy spotting and may occur alongside severe nausea.
A molar pregnancy can often be detected as early as 6–8 weeks through ultrasound and unusually high HCG levels. Early diagnosis helps prevent complications.
Yes, most women can have a healthy pregnancy afterward. Doctors usually recommend waiting 6–12 months and monitoring HCG levels to ensure the molar pregnancy tissue is completely gone.
No, but they can feel similar. A molar pregnancy is not a typical miscarriage- it involves abnormal placental tissue growth. However, both result in pregnancy loss and may require medical treatment.
A molar pregnancy is a rare complication where abnormal tissue grows inside the uterus instead of a healthy embryo. It happens due to abnormal fertilization, leading to the formation of a mass (molar pregnancy tissue) rather than a normal pregnancy.